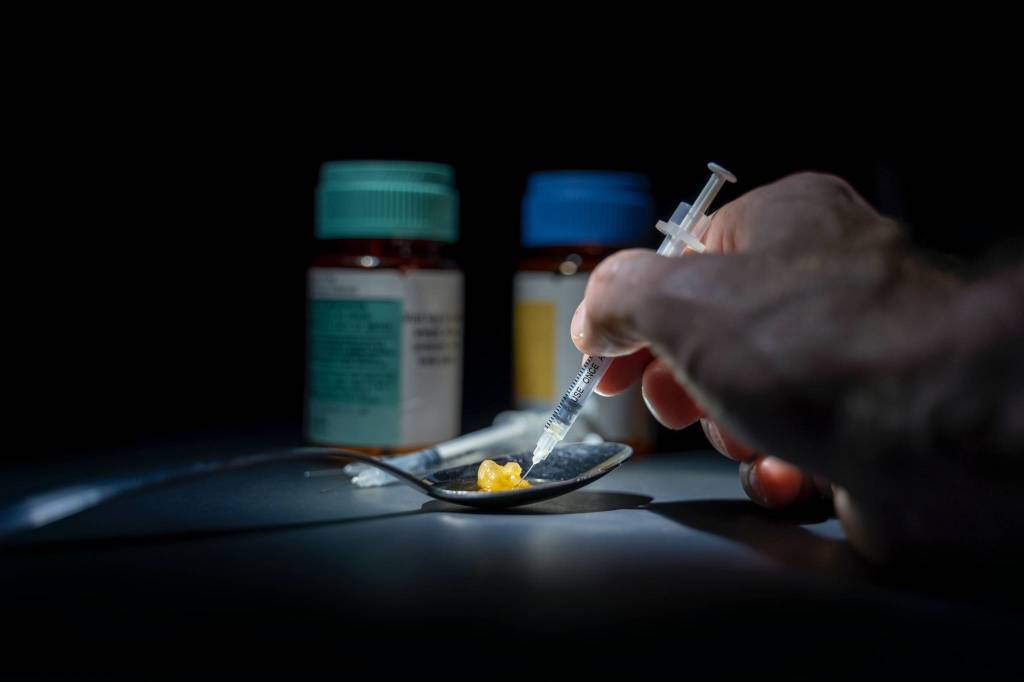
Opinion: What’s happening to substance abuse amid COVID-19
Published 1:30 am Monday, May 11, 2020
We’re all aware of what COVID-19 is at this point. The media have inundated us about the virus, its effects, the deaths. You’d have to be living under a rock to not be a walking statistician about coronavirus by now. But something that isn’t getting much attention is what’s happening with the earlier public health crisis, substance abuse.
Addiction has been America’s epidemic for the last decade, at least. The overprescribing of opioids in the early 2000s fueled and grew the consumption of the drugs, which led to the heroin and fentanyl overdose problems we now see. Millions in funding for treatment and lawsuits against big pharma have been critical points of this battle, as have the growing numbers of lives lost to substance abuse.
COVID-19 arrived early this year, quickly spreading from China to the United States. The news began to shift to the coronavirus and away from the drug epidemic. Programs began being quietly defunded, such as the $4.8 million transferred from substance abuse and mental health problems in late February. The Trump administration decided on this as a way to fund the coronavirus response.
The concern for substance misuse is beginning to emerge as the two epidemics collide, and COVID-19 makes its way to America. March gave way to a 20% increase in overdose emergency calls for the fire and rescue department of Jacksonville, Florida. In the first week of April, the coroner’s office in Columbus, Ohio, saw a spike in overdose deaths as well, with as many as 12 in one 24-hour period. And four counties in New York so far have acknowledged increases in overdose deaths since coronavirus infections have increased in the United States.
But outside of local reports, the CDC has yet to provide national data on overdose deaths during the coronavirus outbreak. Interestingly, one of the biggest obstacles to navigate when COVID-19 first struck was how to handle the administration of opioid abuse medications like Methadone and Suboxone.
Usually given at a clinic, in as little as daily doses. Tight regulation on administration is necessary because these drugs are specialized opioids that still carry abuse potential and overdose risk. Until a patient has a track record of not misusing their medications, they must go to the clinic daily to get their dose. Some patients travel hours to do this, and some clinics see thousands of patients
Shortly after the virus struck America, SAMHSA issued recommendations allowing patients to take home as much as a four-week supply of the drugs. There doesn’t seem to be any data out yet on how medication compliance is going. Meanwhile, Indiana, a state that’s been particularly hard hit by the opioid epidemic, has recently had to issue orders due to the conflict that exists between social distancing measures and drug intervention.
The chief of police in a city near Indianapolis issued orders not to administer Narcan, the lifesaving overdose reversal drug, to apparent opioid overdose patients. His concern is that when revived, the patient may transmit the virus to the first responding officer administering it. Opioids cause respiratory failure, so a drug that suddenly reverses that can cause patients to gasp, cough, and grab at anyone nearby. Instead, he wants officers to stand at least 6 feet away until a medical responder with proper protective equipment arrives. This delay can mean the difference between life and death.
The drug epidemic didn’t just go away.
The two public health emergencies not only collided but are fueling each other. We’ve all experienced the additional stress from COVID-19, with schools and businesses closed, left to do nothing but worry or listen to more bad news. For those in recovery or dependent on substances, this stress can fuel drug use.
A report from University of Southern California brings to light that alcohol consumption has surged with the arrival of the coronavirus, seeing a 55% increase in sales in late March when compared to the same statistic from 2019. And while COVID-19 is fueling substance abuse, those same people are perfect victims of the virus. Drug and alcohol use increase one’s risk of mortality from the virus. Taking all this into account, it’s easy to see that America’s first epidemic hasn’t gotten any prettier and may have gotten worse.
• Joseph Kertis is a health care professional turned journalist. He started his journey in the medical field 10 years ago as a certified nursing assistant for a drug and alcohol rehabilitation center.