Reckoning with the painful legacy of opioids
Published 10:30 pm Thursday, April 7, 2022



Joanna Samson-Sills was first prescribed opioids by a doctor in 2010.
“I just went to him and mainly just did them because they were prescribed to me,” she said. “At first, I didn’t think I had an addiction.”
The oxymorphone pills Samson-Sills took were for her chronic hip and lower back pain. But when her prescription ran out, she looked for painkillers elsewhere.
“When I ran out, of course, I went and got (oxycodone) from random people or morphine pills from random people,” she said. “I liked that it just shut everything off and I didn’t have to deal with any emotions.”
Prescription pills were just one of the controlled substances Samson-Sills struggled with for over a decade. Between 2008 and 2019 the 48-year-old Soldotna resident, who is now in recovery, said she also used alcohol, methamphetamines, cocaine and heroin. But, she said, the opioids played a part in her addiction to other drugs.
“It was like one drug after the other,” she said. “I’d try one drug, and then I’d do so much of it, and I was just sick of it. … And then another drug would be introduced to me, and I’d do that until I got physically sick of it.”
Samson-Sills’ recovery efforts come as people nationwide continue to grapple with the consequences of an epidemic that the U.S. Centers for Disease Control and Prevention estimates has claimed nearly half a million lives due to overdoses between 1999 and 2019.
It’s only been recently, however, that pharmaceutical giants are being made to answer for their role in the crisis. Connecticut-based Purdue Pharma, the creator of the extended-release oxycodone painkiller OxyContin, just last month reached a deal with state attorneys general.
If approved, the company and its owners, the Sacklers, would pay $6 billion to help communities address the opioid crisis. The company pleaded guilty in 2020 to charges related to its marketing of OxyContin.
A bipartisan Congressional report released in February estimates that drug overdoses are currently costing the United States about $1 trillion annually. In 2019, it was estimated that more than 10 million people aged 12 or older had misused opioids in the last year. Of that, an estimated 9.7 million people had misused prescription pain relievers, according to the U.S. Department of Health and Human Services.
The state of Alaska is slated to receive $58 million from a $26 billion nationwide settlement with major pharmaceutical companies Cardinal Health Inc., McKesson Corporation and AmerisourceBergen, as well as Johnson & Johnson.
Of the $58 million coming to Alaska, 15% — about $8.7 million — will go to nine political subdivisions that opted to participate in the settlement, including the Kenai Peninsula Borough. Of that $8.7 million, the borough will get about 9.5% — around $826,500, to be distributed to the borough over 18 years.
The spread of opioids
It was in the mid- to late-2000s that the number of opioid prescriptions began to increase. Nationwide, the total number of opioid prescriptions dispensed grew from about 216 million in 2006, to about 238 million in 2008, to about 251 million in 2010, according to the CDC.
Cardinal Health, McKesson Corp. and AmerisourceBergen were the top three opioid distributors in Alaska between 2006 and 2014, according to a database maintained by the Drug Enforcement Administration, which was made public by The Washington Post and tracks shipments of oxycodone and hydrocodone pills.
On the Kenai Peninsula, almost 22.5 million hydrocodone and oxycodone pain pills were supplied to the borough between 2006 and 2014. That’s compared to the almost 183 million prescription pain pills distributed statewide during that time.
Soldotna Professional Pharmacy, which is co-owned and operated by Justin Ruffridge, received almost 5.15 million of those doses between 2006 and 2015. Ruffridge recalls an attitude of complacency among health care professionals as he first entered the field, specifically as it related to “conquer(ing)” pain through the use of novel prescription pain medication.
“There was a common theme during my tenure in school that nobody should live in pain,” Ruffridge said. “On its face, that sounds really great.”
As reported by NPR, the companies named in the settlement did not acknowledge wrongdoing for their role in manufacturing and distributing large amounts of pain medication when opioid addiction and overdoses were increasing.
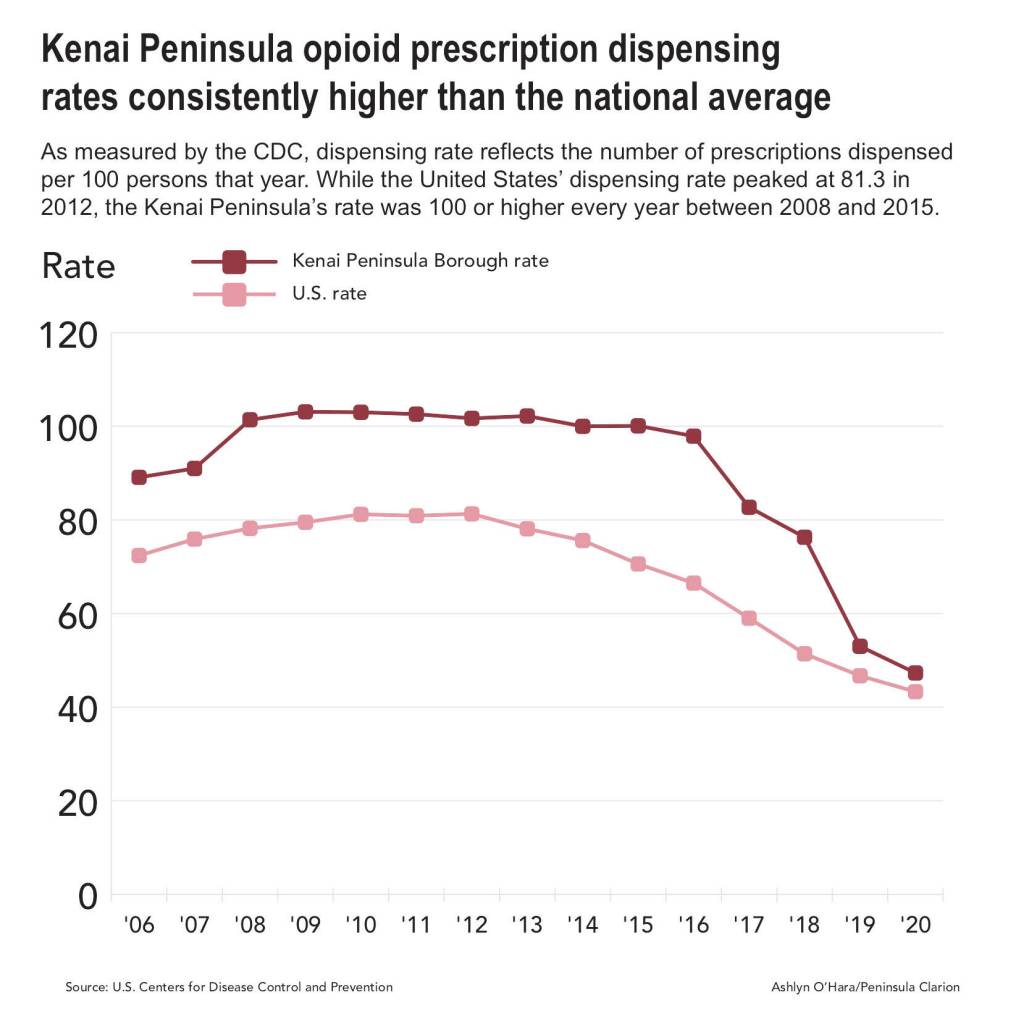
Opioid prescription dispensing rates on the Kenai Peninsula were consistently higher than the rest of the country between 2006 and 2020. As measured by the CDC, dispensing rate reflects the number of prescriptions dispensed per 100 persons that year. While the United States’ dispensing rate peaked at 81.3 in 2012, the Kenai Peninsula’s rate was 100 or higher every year between 2008 and 2015.
During that time, the estimated rate of opioid prescriptions dispensed per 100 residents in the Kenai Peninsula Borough did not drop below 100, according to the CDC. The rate of opioid prescription dispensing was higher on the Kenai Peninsula than in the United States as a whole from 2006 to 2020, according to CDC data. Nationwide, that rate never went above 100.
“It was in 2014 and 2015 when people in this area started to say, ‘We have a problem,’” Ruffridge said of the central peninsula.
Community members, including parents, began to raise concerns. Ruffridge described early pushes to raise awareness about substance abuse as a “concerted effort” by people in the community, who he said were “tired of finding their loved ones had overdosed, often with irreversible outcomes.”
According to the National Institute on Drug Abuse, more than one in five patients — between 21% and 29% — prescribed opioids for chronic pain misuse them. Between 8% and 12% of people using opioids for chronic pain develop an opioid use disorder.
Between 2010 and 2017, the opioid overdose death rate increased by 77% in the state of Alaska, according to the Alaska Department of Health and Social Services. Like the United States as a whole, Alaska saw the highest number of deaths related to opioids in 2017: 108 deaths were reported in Alaska that year, about 93% of which were due to overdose.
DHSS reports on its opioids webpage that “progress is being made.” Use of naloxone, commonly sold under the brand name Narcan, is medication used to rapidly reverse an opioid overdose. Naloxone use is increasing, DHSS reports, which it attributes to increased availability statewide.
Additionally, the number of people who die each year due to opioid overdoses is going down and the rate of Medicare Part D patients who received opioid prescriptions has decreased every year since 2015.
‘It’s not a choice’
Originally from Oregon, Samson-Sills was sent to live with her grandparents in Alaska as a child. While she was young, she said she experienced abuse and unstable living conditions.
As she got older, Samson-Sills said she started by drinking alcohol occasionally “to fit in.” Then, she said, she started experimenting with other drugs, including opioids, because people around her were using.
“And then it just got to the point where, I don’t know what happened,” Samson-Sills said. “It’s just like an everyday thing to live.”
She said a major turning point was in 2012, when she went to jail for the first time as a result of her addiction.
“I knew I didn’t want that life, and I didn’t know how to get out of it,” Samson-Sills said. “I prayed to God that he would take everything from me, all that addiction. Because I never wanted to use, it was just a need.”
Samson-Sills recalled a visceral response to her prayers — her body felt cold, even bloated at times, like it was purging out of necessity so it didn’t decompose completely.
“I wasn’t alive, but I wasn’t dead,” she said. “I was walking in a daze. It’s like time stood still.”
She began addiction treatment later in 2012 at the Serenity House Treatment Center in Soldotna, where she experienced more enlightenment. She said she felt joy for the first time then, when she was 38 years old.
But Samson-Sills got in trouble with the law again, she said, this time landing in prison. Soon after she got out in November 2013, her mother died and she relapsed with heroin. She became entangled with the legal system another time, and went back to Wildwood Correctional Complex in 2019, where she realized she had a real problem.
“In between 2013 and the time I got arrested in 2019, I realized I (was) into opiates,” Samson-Sills said. “Because I really wasn’t a methamphetamine user, once in a while I did it, but that wasn’t mine. It was either the pills or the opiates.”
The word opioid can be used to describe natural, semisynthetic and synthetic opioids, according to the CDC. The word opiate refers to natural opioids, such as heroin and morphine, that are derived directly from the poppy plant.
Samson-Sills emphasized the need to treat pain without using potent painkillers, and said it’s not always necessary for health care providers to prescribe opioids.
“Pain is manageable without medication,” Samson-Sills said. “There’s other ways. The doctors don’t just have to dish them out for pain.”
She most recently left incarceration with an ankle monitor in October of last year. She’s been out on parole since December 2021.
Samson-Sills said she wants to make one thing clear: that the drug and opioid crisis can’t be learned “the standard textbook way.”
“We’re not born addicts, you know, and they look at people like junkies and all this stuff, and we’re not,” Samson-Sills said. “It’s not a choice.”
The relationship between opioids and other street drugs, such as heroin, has been well established. Between 4% and 6% of people who misuse prescription opioids transition to heroin, and about 80% of people who use heroin first misused prescription opioids, according to the National Institutes of Health.
Rheanna Tussey didn’t use prescription opioids, but she did seek help from the Cook Inlet Council on Alcohol and Drug Abuse after struggling with heroin use for about six years.
The 28-year-old Kenai resident described going to a “dark” place after multiple hardships during her young adulthood in Homer — including her boyfriend’s death by suicide and the loss of her job and house — and wound up incarcerated for things she did while under the influence of heroin.
“I knew I needed help,” she said. “It was either I was going to wind up dead or in jail.”
Tussey said her experiences with heroin probably weren’t different from those of other opioid addicts. Looking back, she said even her grandfather was probably abusing his prescription pain pills.
“It’s like, how can you judge me on what I’m doing when you’re doing it but in a different version?” Tussey said. “Everything was taboo, but it’s all the same. All the opioids are the same.”
The fallout
In the years since the epidemic peaked, Ruffridge said he has often thought about his role as a pharmacist and questioned how he and other pharmacists could do more. He once asked someone in recovery if there was something he should have done differently as a pharmacist if he suspected opiate misuse, but was told that hope for change must start with the person struggling with dependency.
A lot has changed since the epidemic’s height on the peninsula, Ruffridge said. Notably, there’s more pharmacist counseling involved when it comes to opioids. If he suspects someone picking up a prescription for a controlled substance may be struggling with dependency, he said he usually goes back to the prescriber to voice his concerns and provides face-to-face counseling on how to use opiates safely.
Ruffridge said treatment has become well rounded. It’s now common to ask if the patient has considered alternative ways of treating pain, such as physical therapy or acupuncture.
Narcan is often dispensed with opioids. Pharmacists in Alaska are able to dispense naloxone independently of prescribers. The National Institutes of Health describes naloxone as an “opioid antagonist,” meaning it attaches to opioid receptors and reverses and blocks the effects of other opioids.
Shari Conner, who works at Central Peninsula Hospital, told a group of volunteers at a Narcan workshop at the Freedom House last year to think of opioids like tiny golf balls and someone’s neuron receptors like golf tees. As long as the opioid is active, it sits on the “tee” of someone’s receptors. When the opioid dies, it falls off the receptor and new opioids stick on them. Naloxone knocks all the opioids off their receptor tees.
The drug only has a half-life of about 30 minutes, however. Once it starts dying, opioids rush to fill those tees back up. That’s why it’s so important for the person responding to the overdose to call 911.
According to the CDC, signs of an opioid overdose include loss of consciousness, slow or shallow breathing, pale or blue skin, a limp body and constricted pupils, among others. The CDC instructs that if you find someone who you think is overdosing, call 911 immediately.
Looking ahead, Ruffridge said there’s still work to be done. Generally, he thinks more empathy is needed as community members consider how to address the problem of drug dependency. A reduction in stigma and an understanding of the “soul-crushing shame” many addicts struggle with can go a long way.
“We treat people that have a drug issue really poorly,” Ruffridge said. “ … There is a lot of misunderstanding about what it feels like and what it looks like to be dependent on a drug.”
As the Kenai Peninsula Borough moves forward with accepting and allocating opioid settlement funds, Ruffridge said he would love to be a part of the process. He hasn’t been asked to participate yet, but said he’s willing and able when the time comes.
The settlement
As part of the settlement, Johnson & Johnson will not fund or provide grants to third parties for promoting opioids and not lobby related to opioids. The company will also not resume selling opioids, which it stopped doing nationwide last year.
Cardinal Health Inc., McKesson Corp. and AmerisourceBergen will, among other things, use data to detect suspicious opioid orders from customer pharmacies, prohibit the shipping of and report suspicious opioid orders and require senior officials to engage in regular oversight of anti-diversion efforts.
The companies will also be required to establish a central and independent clearinghouse that will provide all distributors with data and analytics about where drugs are going and how often, the Alaska Department of Law said in a March 1 press release. That effort will eliminate “blind spots” in the system currently used by distributors, the department said.
The borough’s settlement money will be paid out over the next 18 years, according to Kenai Peninsula Borough Attorney Sean Kelley, who said the borough is expecting to receive about $46,000 per year. Still, nothing is set in stone. About 70% of the $58 million coming to Alaska, Kelley said, will go to Alaska’s Opioid Abatement Accounts Fund.
Kelley said it is anticipated that legislation will be put before the assembly in the coming months that will formally kick off a public process regarding how funds should be handled and distributed. Funds received must be used for opioid remediation as outlined in the Final Distributor Settlement Agreement, though exactly what type of remediation is up to the receiving entity.
The Alaska Department of Law said that Gov. Mike Dunleavy’s Advisory Council on Opioid Remediation will make recommendations about how the money should be spent, with a report to Dunleavy due Dec. 1. That council consists of 13 members representing local government, public health and state lawmakers.
Around the peninsula, people have different ideas about how the borough’s settlement money should be spent.
Treatment evolves
Annette Hubbard is the medication assisted treatment program case manager at the Ninilchik Traditional Council’s Community Clinic, which specializes in innovative addiction treatment services. She thinks borough funding should be put toward creating more transitional sober living spaces on the peninsula, as well as hiring more health care providers to educate people about substance use recovery and treatment.
The clinic’s medication assisted treatment program is recognized both statewide and nationally, she said. Part of the regimen includes offering buprenorphine injections to people struggling with addiction, as well as a daily prescription of the drug, and consulting with other addiction treatment facilities across the state.
Buprenorphine is described by the U.S. Department of Health & Human Services’ Substance Abuse and Mental Health Services Administration as an opioid partial antagonist that can be used to treat opioid use disorder. When taken as prescribed, the agency says, buprenorphine can diminish the effects of physical opioid dependence, such as withdrawal.
What makes the program unique is its approach to addiction treatment. Instead of solely pushing abstinence-based treatments, Hubbard said the clinic also works to educate patients on how they can reduce their risk. That approach is referred to as harm reduction, which Hubbard described as “how to do unsafe things safer.”
Unlike traditional addiction treatment models, Hubbard said the goal isn’t always for a patient to quit substance use altogether. Instead, the team tries to create a plan that works for each individual, such as offering walk-in appointments and counseling services.
“We can’t tell you what to do, but we can give you education,” Hubbard said. “You have to do a treatment plan that’s going to work for them, that they know they can adhere to.”
Many patients, she said, aren’t trying to seriously harm themselves while using substances.
“That’s not what they’re trying to do, they’re just trying to get their house clean or they’re just trying to get out of bed,” Hubbard said.
Hubbard sought treatment at a similar program as a patient in 2009, when she herself struggled with alcohol use. Prior to joining the clinic as an employee, she spent six years working for the Alaska Psychiatric Institute, where she said she realized how difficult it was for patients, particularly in rural and tribal communities, to access services.
“Seeing how people in rural communities weren’t able to access behavioral health for whatever reason … that kind of was really disheartening,” Hubbard said.
As the borough prepares to plan the distribution of settlement funds across the peninsula, Hubbard said it should keep those questions about accessibility in mind.
“Why are people coming from Kenai and Soldotna and Seward when there are primary care clinics in their community?” she said. “The homeless shelter out in Nikiski isn’t going to work for everybody in Homer, how are they going to get there?”
In the meantime, Hubbard said, the opioid crisis is far from over. In fact, she said, right now the area is “in the peak.”
The drugs being used now are especially dangerous because of their potential to be laced with fentanyl, a synthetic opioid that the DEA says is between 80 and 100 times stronger than morphine.
DHSS reported Friday a “sharp increase” in overdose deaths in 2021, which it attributed to the rise in fentanyl use. The number of drug overdose deaths increased by 68% over the course of one year, the department said, from 146 drug overdose deaths in 2020 to 245 in 2021. Last year, 140 drug fentanyl overdose deaths were reported in Alaska. Of those, 61% also involved methamphetamine and 28% also involved heroin.
“Opiates (are) a different breed, because we know that will kill you,” Hubbard said. “Methamphetamines right now are definitely laced with fentanyl.”
Fentanyl is a synthetic opioid that is approved for treatment of severe pain. Fentanyl that is illegally made, however, is what’s linked to “most” recent cases of fentanyl harm, overdose and death, the CDC said.
Hubbard emphasized that opioids “affect everybody” regardless of demographics, and that people who struggle with substance use deserve more grace.
“They’re not bad people, everything is out of necessity,” she said. “We’ve got to give people a chance … We need more providers, and just people in general to be compassionate and not stigmatizing.”
Resources
Mario Madera is a house leader at Acts 247 Recovery Church in Kasilof. He’s a recovering addict who said he was visited by an angel in 2008 who helped him turn to God and get clean.
“God just changed me,” Madera said.
Since moving to Alaska the same year, he’s opened his home to people in similar circumstances. Madera would like to see some of the settlement money coming to the borough be used for a starter home, which he described as a place people can stay to get off the street as they wait for spaces in other facilities to open.
“All I wanted while I was on the streets and using was a chance,” Madera said.
A starter home would differ from places like the Nikiski Shelter of Hope, which offers conditional temporary housing to qualified applicants. If a starter home opened on the central peninsula, Madera said, he’d quit his job to help operate it. The Nikiski shelter opened in December and has since assisted 32 people, including 22 adults and 10 children, according to Love INC Executive Director Leslie Rohr.
“We’ve got people out here who want to get clean and sober but they just don’t have a place to go,” Madera said.
Like Ruffridge, Madera said a key aspect of opioid remediation will be showing compassion for those struggling and going through recovery.
“I really just believe caring and love is going to break the cycle around here,” Madera said.
Others in recovery echoed similar sentiments.
All things considered, Tussey said doing jail time made her reflect on her life. She decided to seek treatment at the Cook Inlet Council on Alcohol and Drug Abuse in Kenai when she got out.
“I wanted to be a contributing member of society again,” she said. “I only got one life and this is not the way I want to live it.”
Tussey said the larger community needs to be aware of the realities faced by those struggling with addiction. Out on adult parole, Tussey just hit her eight-month sobriety mark. She got a job on the central peninsula, and a car, and is going to move into a bigger house soon.
“It’s one of those things where no matter what, everybody has their poison,” she said. “Everybody makes bad decisions, you can’t judge somebody on their past. You can help them move forward.”
At Soldotna’s faith-based sober living unit Freedom House, Samson-Sills makes sure everyone is accounted for by curfew every night. Officially she works there as the night manager, but unofficially she’s the “house mom.”
In between work, Samson-Sills is also studying for a bachelor’s degree in psychology through the Florida Institute of Technology online with the hopes of becoming a trauma mentor. She said she has a good relationship with her children.
Samson-Sills said the journey toward recovery is worth it. As she reflected on the most rewarding parts of her own progress, she said finding God and finding a home at the Freedom House have made all the difference.
“It makes me want to cry just thinking about it,” she said. “ … You’re accepted, you’re wanted, you’re loved, you’re cared for. We all want a place in this world and (to) feel that. You get that sense of peace and just overwhelming happiness and joy that someone truly cares for you, that you matter in this world.”
If you or someone you love is struggling with substance use, consider reaching out to one of the peninsula’s addiction treatment and recovery centers.
Emergency dispatch: 911
Freedom House sober living, Soldotna: 907-260-3733
Serenity House Treatment Center, Soldotna: 907-714-4521
Cook Inlet Council on Alcohol and Drug Abuse, Kenai: 907-283-3658
Cook Inlet Council on Alcohol and Drug Abuse, Homer: 907-235-8001
Ninilchik Traditional Council Community Clinic, Ninilchik: 907-567-3970
Homer Needle Exchange, South Peninsula Hospital, Homer: 907-235-3436
SeaView Community Services, Seward: 907-224-5257
Reach reporters Ashlyn O’Hara and Camille Botello at ashlyn.ohara@cmg-northwest2.go-vip.net/peninsulaclarion and camille.botello@cmg-northwest2.go-vip.net/peninsulaclarion.