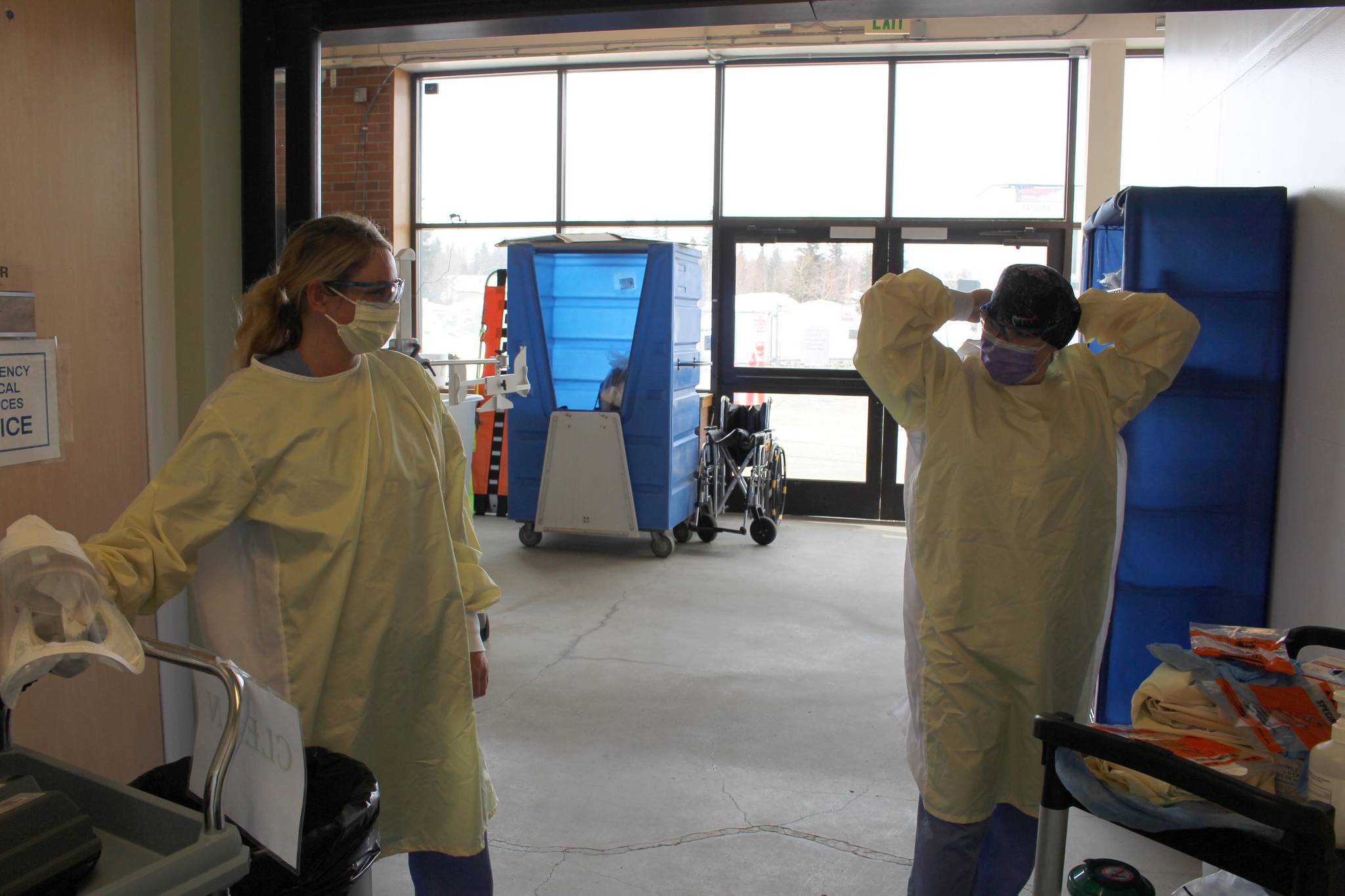
As rising COVID-19 cases strain hospitals across the state, Central Peninsula Hospital reported Thursday that it has almost reached capacity.
Bruce Richards, CPH external affairs director, said the hospital has 49 beds, including 34 medical/surgical beds and nine ICU beds. The rest are obstetric unit beds, four of which are flex beds that the hospital can use if needed.
As of Thursday morning, Richards said, there are 36 medical/surgical beds in use and seven ICU beds in use.
“We’re basically full, with the exception of a few OB beds,” Richards said. “We’ve been running pretty close to capacity for a while. It’s not uncommon — it ebbs and flows — but we do have six COVID-positive patients.”
Statewide, there were 120 people hospitalized on Thursday who were COVID-19 positive or considered persons under investigation for the disease.
Richards said CPH will benefit from Gov. Mike Dunleavy’s new disaster declaration, which takes effect Monday, because it lessens the amount of red tape they normally deal with, such as the number of licensed beds they are allowed to have.
Richards said that the high number of patients being treated at CPH is a sum of several factors. Since the beginning of the pandemic, CPH has had hardly any COVID-19 patients and treated maybe one or two at a time. A few days ago, Richards said, they were treating eight COVID-19-positive patients.
“It’s definitely increased in the last two weeks,” Richards said. “Obviously, there’s a huge spike in the positive numbers locally … we’ve set records the last few days as far as positive cases and we’re definitely seeing that.”
At an Alaska State Hospital and Nursing Home Association press conference on Nov. 6, CPH CEO Rick Davis spoke about the personnel shortage that CPH and hospitals nationwide are experiencing.
Richards said that as of Thursday morning, 76 of CPH’s approximate 1,000 staff members were in quarantine because they had either tested positive or were identified as a close contact of someone who tested positive. CPH really feels the loss of employees, Richards said, because every employee is important.
“They all have a specific job at the hospital and once that starts getting impacted your efficiency starts to go down,” Richards said. “It makes it harder for some places where things are hit harder and maybe in one department you have people that are working longer shifts.”
The shortage has not been helped by an outbreak at Heritage Place Skilled Nursing facility, which was announced on Nov. 8. Between Oct. 26 and Nov. 8, seven people tested positive for COVID-19 at Heritage Place, including three residents and four staff. As of Thursday, there were four positive residents at Heritage Place.
Richards said part of the trouble is in trying to curb community spread, which he said can be done if people do simple things like wearing a mask, social distancing and not going places where they don’t need to.
“You can keep the economy going and everything else by doing a few of these things, but right now that’s not happening and we’re seeing a spike,” Richards said.
If the number of patients continues to increase and the number of hospital staff able to work continues to decrease, Richards said, employees will have to take on more patients. Richards said that he doesn’t know if CPH would ever get to that point, but that they have difficulty bringing up replacement workers from the Lower 48. He said this difficulty is caused in part by trying to get people to move to Alaska in the winter and in part due to a nationwide shortage of workers.
“There’s a huge spike going on across the country,” Richards said. “We’re setting daily records and so there’s fierce competition for these personnel.”
All plans related to COVID-19 vaccine developments are being handled at the state level, Richards said.
As of Thursday morning, there are more than 1,000 active COVID-19 cases on the Kenai Peninsula, according to the Alaska Department of Health and Social Services. On Thursday, the state recorded a daily COVID-19 case increase of more than 450 for the seventh day in a row.
Reach reporter Ashlyn O’Hara at ashlyn.ohara@peninsulaclarion.com.