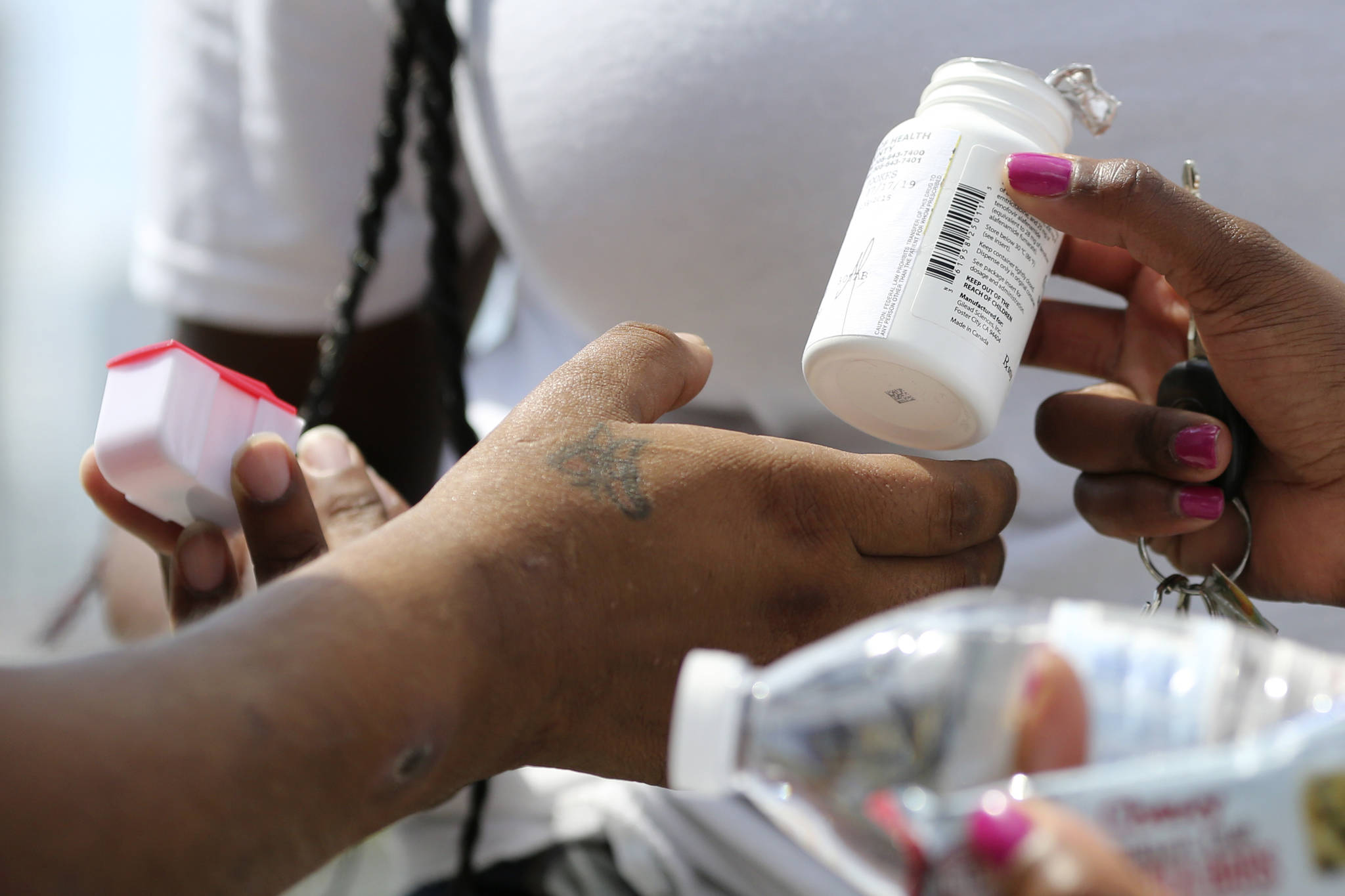Alaska’s nation-leading rates of sexually transmitted disease transmission aren’t matched by a high rate of new HIV cases, according to state data.
Alaska had the highest rate of chlamydia in the country, and the second-highest rate of gonorrhea, according to the Centers for Disease Control and Prevention’s most recent STD surveillance report released in early October. Data from the state’s Section of Epidemiology show 22 new cases of HIV were diagnosed in Alaska last year. That’s low by national standards and typical for Alaska. In 2017, the national rate was 14 cases per 100,000 people. In Alaska, the rate was 4.8 per 100,000 people.
“We have between 20 and 50 new HIV cases every year, and that has been really consistent the last 10 or 15 years,” said Susan Jones, HIV/STD program manager for the State of Alaska Section of Epidemiology.
Jones said Alaska has typically been considered a “low incidence” state for HIV. There is a known “cluster” of HIV cases in Fairbanks, but Alaska continues to be a state where HIV transmission is relatively uncommon.
Alison Gaines, nurse manager for Juneau Public Health Center, said local trends seem to be in line with state data, which shows low incidence of HIV.
“There’s a lot of contributing factors behind that,” Jones said.
One of the main contributors, Jones said, are modern anti-viral medications that can suppress HIV to undetectable levels. Sustained viral suppression means it’s less likely the virus will be transmitted to others.
“If you have sustained, usually about six months worth, of viral suppression, and it stays that way, the risk of you transmitting HIV through sexual contact is zero,” Jones said.
[Syringe exchange in danger of going under]
Encouraging treatment to reduce transmission of HIV is the focus of the national U=U (Undetectable Equals Untransmittable) Campaign, an effort to raise awareness of the connection between viral suppression and reduced risk of transmission.
According to state statistics, 564 of the 699 people in Alaska living with HIV are virally suppressed, and 635 are receiving some sort of medical care.
There’s another reason Alaska can have a history of both low HIV instances and high STD transmission rates.
Jones said while STDs and HIV can be transmitted in the same way, they’re spread among populations with different demographics. That means chlamydia and gonorrhea can be transmitted among distinct “sexual networks” — groups of people linked by a common sexual partner — which helps explain a difference in transmission rates.
She said in Alaska, men who have sex with men, are the primary mode of HIV transmission. According to state data, 55% of Alaska residents with HIV — 386 of 699 total — are men who have sex with men, and 75% — 524 of 699 — are men.
As a comparison, 64% of chlamydia cases reported to the Section of Epidemiology — 3,975 of 6,173 — were in women.
While HIV and STD rates are different, they’re not totally unrelated. Gaines said those who contract a STD are more likely to be HIV positive.
Jones said there are some tools people who engage in risky behavior, such as having multiple, relatively anonymous sexual partners, or using intravenous drugs, have at their disposal to limit risk of contracting HIV.
Those include using some sort of latex barrier when engaging in sexual behavior and using clean needles if injecting drugs.
Pre-Exposure Prophylaxis (PrEP) is another tool, Jones said. PrEP is a pill taken daily that can protect people from HIV.
“The medication is really pretty easy to take every day,” Jones said. “The side effects are quite minimal.”
[Ceramics are messy, time-consuming and loved by this Juneau artist]
However, she said it may not be easy to get for people without insurance.
In order to be taking PrEP, a person must test negative for HIV and be tested every three months to ensure they’re still negative. Without insurance, Jones said that can be cost prohibitive, even with assistance programs that can subsidize the cost of the medication.
Regular testing is a good idea for people who may be at risk for HIV or STDs regardless of whether they wish to obtain PrEP, Jones and Gaines said.
A history of negative tests followed by a positive test can help determine when HIV was contracted and help get people appropriate care, Jones said.
“It helps us in public health to know when your last negative test was,” she said.
State resources
The statewide AIDS helpline is 1-800-478-2437.
A list of HIV testing locations can be found through gettested.cdc.gov.
At-home testing kits can be ordered through iknowmine.org.
• Contact reporter Ben Hohenstatt at (907)523-2243 or bhohenstatt@juneauempire.com. Follow him on Twitter at @BenHohenstatt.